Table of Content
To ensure fair comparison of serious illness programs, quality measure scores should be case-mix adjusted for variables that influence patients' reports about care quality, but are not under the control of the program administering care. As part of a national effort to develop palliative care quality metrics for use in accountability programs, we sought to develop survey items assessing patients' experiences of outpatient palliative care, incorporating the patient's voice. For the beginning, you can start by following these two marketing key performance indicators for home health care we’ve selected.

This page contains brief descriptions of each measure type and how the data for that measure is calculated. TheDownloadssection below provides links to technical documentation, tables identifying which Home Health Quality Measures are risk-adjusted and reported publicly, and additional resources. Evidence shows that leaders who implement the patient-centered medical home care model encounter challenges in driving change. Understanding which changes and quality improvement practices further implementation is essential. The Agency for Healthcare Research and Quality held a research meeting on using Consumer Assessment of Healthcare Providers and Systems (CAHPS®) data for quality improvement and evaluating such efforts.
Which KPIs Should Your Home Health Care Agency Track?
The purpose of this paper is to examine the content and actionability of written comments from parents and guardians on the Child Hospital Consumer Assessment of Healthcare Providers and Systems survey. Programs offered at an independent public policy research organization—the RAND Corporation. A decision on which KPIs your agency will track and how deep in the metrics you’re willing to go will depend primarily on your business organizational priorities and tangible goals. Certain software solutions, such as Timeero, can help you keep track of essential KPIs smoothly so that you can act upon the findings timely. You can track changes in this KPI to determine if, for example, your marketing strategies are working or how the price changes affect the demand for your services.

To calculate it, divide the number of clients admitted by the total number of people who made an inquiry about your services in the same period. If the client turnover is significant, it might imply poor client satisfaction and the low quality of the service provided. You can calculate it by dividing the number of all active clients during a time period by the number of months care was provided.
Alignment of quality indicators with broader home care reforms
By tracking the following key performance indicators for home health care, you can identify the problems early, and take appropriate measures. To keep your agency's performance at a high level, you need to ensure that the services you’re providing are being delivered according to your client’s personal needs, at the right place, and at the right time. Below you will find four key performance indicators in healthcare that fall into this section, that you might benefit from tracking. In accordance with Government decision to align the introduction of quality indicators with broader home care reforms, work of the consortium has refocused to identify, assess and deliver an operational framework for quality indicators and CEQOL measures in a new in-home aged care program. Our analyses provide evidence of the feasibility, reliability, and validity of proposed survey-based measures to assess the quality of home-based serious illness care from the perspective of patients and their families. Regarding key performance indicators for home health care, they should cover all key areas like overall client satisfaction, on-time client visits, employee retention, reporting, and billing.
The objective was to conduct a systematic review of toolkit evaluations intended to spread interventions to improve healthcare quality. We aimed to determine the components, uptake, and effectiveness of publicly available toolkits. Besides financial profit drivers, such as price or service volume, non-financial profit drivers are also significant to consider. They include customer satisfaction, productivity, service quality, employee satisfaction, etc. Some of these drivers are mentioned above and below, as key performance indicators for home health care.
Events
Despite efforts by insurance companies and other payers to move toward compensating physicians based on the quality and value of care they provide, most physicians employed in group practices owned by health systems are paid primarily based on the volume of care they provide. Drawing upon decades of experience, RAND provides research services, systematic analysis, and innovative thinking to a global clientele that includes government agencies, foundations, and private-sector firms. Over time, it may indicate whether your agency is understaffed, leading your caregivers to burnout and reducing the quality of service, or overstaffed, causing too high overhead expenses. Calculate this KPI by dividing the number of clients that stopped services during a specific period by the total number of clients with the agency during the same time period.
This paper presents evidence that the quality of health care interactions changed in important ways during the early months of the Covid-19 pandemic. We surveyed children's hospital leaders and staff about their use of Child HCAHPS for QI, including measures from other studies. We compared scale and item means for leaders and staff and compared means to other studies. In 2008–2017, 15–18% of U.S. primary care practices sought or maintained patient-centered medical home recognition. We interviewed a sample of 105 of these practices to determine why patient experience surveys were chosen. Depression, PTSD, traumatic brain injury, and substance use disorders interfere with veterans' employment, family life, community engagement, and well-being.
What Parents Have to Say: Content and Actionability of Narrative Comments from Child HCAHPS Survey
The data collected by tracking KPIs provides statistics and enables a home healthcare agency to analyze its progress over a specific time, compare it to its industry peers and look for ways to improve its performance. The National Quality Forum , a multistakeholder organization established to standardize health care quality measurement and reporting, has endorsed several consensus standards for skilled home health services. Process measures evaluate the rate of home health agency use of specific evidence-based processes of care. The HH process measures focus on high-risk, high-volume, problem-prone areas for home health care. These include measures pertaining to all or most home care patients, such as timeliness of home care admission.
This way, you can develop effective strategies to maximize your profit and achieve better growth results. They usually consist of rent, utilities, employee salaries, insurance, taxes, professional services, marketing, advertising, technologies, and more. Agencies that are not CMS-certified can develop their own surveys to establish client satisfaction and determine their own strengths or weaknesses. These criteria can help you narrow down the KPIs, producing more effective performance measures.
We would, in effect, be carrying out a targeted and focused sampling of the care provided. So rather than developing long lists of indicators to assess every aspect of care, we should ask how many indicators are needed to make a reasonable assessment of a specific underlying construct. If the indicator set covers multiple constructs , then we should look for redundancy within rather than across these domains, as we still need content validity for each of these constructs. The purpose, broadly speaking, of all indicators is to monitor and hopefully improve the quality and value of care provided in the health system.
The Centers for Medicare & Medicaid's Services reports many of the NQF-endorsed measures on its Home Health Compare website. Some other report developers also present this data, sometimes along with other information about home health care. For a list of home health outcome measures, please refer to the Home Health Outcome Measures Table, which can be located via the link for Home Health Measures Tables in theDownloadssection below. Technical Specifications for calculating OASIS-based outcome measures, patient-related characteristics measures, and the factors used to risk adjust outcome measures, can be accessed via the link for Technical Documentation of OASIS-Based Measures in theDownloadssection below.
A set of standards can help identify providers who serve veterans and deliver high-quality care. Such analysis can help you determine whether there is anything in the process that makes the prospective clients give up using your agency's services. By tracking KPIs for your primary goals, you will know if your team is reaching home health productivity benchmarks, and you can implement incentives based on their achievements.
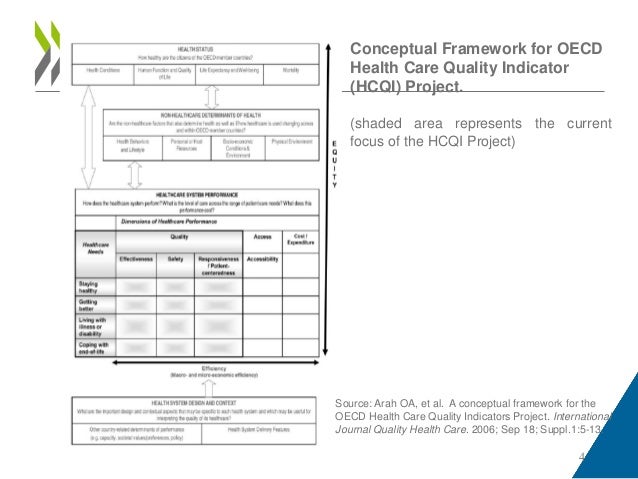
This population-based cross-sectional study found that although quality of care and patient experience were slightly higher with higher-premium plans, quality varied widely within each premium category. The list of key performance indicators for home health care we’ve suggested is essential but far from final. This post walks you through 12 of the most common key performance indicators for home health care. The list is categorized by the Institute of Medicine’s domains for a quality health care system; for definitions, go to The Six Domains of Health Care Quality. However, measures for home health currently focus on only three of the IOM categories; measures in development address additional areas, with an emphasis on patient-centeredness.

No comments:
Post a Comment